A Review on home oxygen therapy (HOT) in severe chronic obstructive pulmonary disease (COPD) patients with resting Hypoxemia
Nada A Alsaleh1,2
1 Department of Pharmacy Practice, College of Pharmacy, Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia. 2 Strathclyde Institute of Pharmacy and Biomedical Sciences, University of Strathclyde, 161 Cathedral Street, Glasgow, G4 0RE.
ABSTRACT
Home oxygen therapy - often abbreviated as HOT - refers to the basic treatment used among patients with acute chronic obstructive pulmonary disease (COPD). The treatment is suitable for use among patients with resting hypoxemia. The objective of this research was to assess the risks, adherence, benefits, as well as the perception of HOT. The primary risk identified in this research relates to burns developing among patients on HOT. In all the studies included in this review, the most popular reason for burns was smoking while on HOT. It is clear from this study that HOT increased the rate of survival among COPD patients diagnosed with mild to moderate and acute hypoxemia. This research recommends the need for more investigation to be carried out to identify additional benefits of participating in HOT. It was evident that patients who were trained on HOT clearly understood the benefits of oxygen and had a superior rate of adherence to this form of treatment compared to those who did not receive any form of training. The outcome of most studies showed positive experiences among patients on HOT. However, the experiences of the patients differed and a few of them reported having negative perceptions. In general, additional scholarly work is needed to examine the thoughts of the patients on HOT and the factors allied to those perceptions. This study can be useful in improving the clinical practice of HOT.
Keywords: home oxygen therapy; benefits; domiciliary oxygen; HOT; risk; adherence.
Introduction
Health is very important to us [1]. Oxygen therapy which is referred to as supplemental oxygen is important for various reasons [2]. To begin with, treatment procedures for lung disease have largely relied on oxygen therapy ever since 1992 [3]. This treatment procedure has also been used for patients suffering from cardiac or neurological disease, such as cluster headaches. Additionally, the success of palliative medicine largely depends on oxygen therapy. At times, patients can receive oxygen treatment at home in what is referred to as home oxygen therapy (HOT) or rather domiciliary oxygen. HOT may be recommended to a patient for several reasons as illustrated in Figure 1. The success rate of oxygen therapy has been examined in many empirical studies. For instance, a randomized controlled trial (RCT) carried out in the UK several years ago demonstrated the power of long-term oxygen therapy (LTOT). Specifically, LTOT implemented under particular conditions enhanced the rate of survival among patients diagnosed with chronic obstructive pulmonary disease (COPD) [4]. Ever since the findings of the RCT were made public, HOT has become a popular treatment procedure. An estimated 85,000 patients get HOT prescriptions in England, among which 60% are diagnosed with COPD. Besides, the National Health Service (NHS) spends more than £100 million annually on oxygen service, which is a remarkable increase since 2005. In London alone, the government spends about £12 million a year on an estimated 11,000 patients on oxygen. Most of these patients are either diagnosed with COPD or other diseases affecting the respiratory system, such as chest wall deformity, interstitial lung disease, or pulmonary hypertension [5]. Since the use of HOT has been on the rise in recent times, it is important to have clear information on the gains, consequences, perceptions of, and adherence to this form of treatment.
Healthcare practitioners can recommend any of the following four classes of oxygen therapy to patients at home [6]:
- Long-term oxygen therapy (LTOT) – LTOT is used when a patient needs constant and continuing treatment. For this therapy to be successful, oxygen must be used at home for at least 15 hours each day.
- Short-burst– Under this therapy, a patient uses oxygen at home occasionally for short durations. Some of the scenarios where this treatment could be used include before or after exercise or rather when a patient needs to alleviate breathlessness.
- Ambulatory– This form of treatment is movable and is often used to support patients who need oxygen therapy besides the home.
- Nocturnal– This treatment procedure is used on patients who need oxygen at home during the night.
Some authors have recognized home oxygen therapy as synonymous with long-term oxygen therapy as well as continuous oxygen therapy.
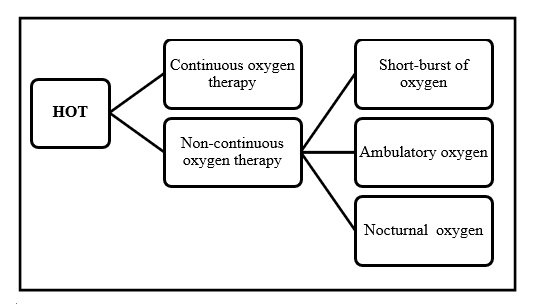
Figure 1. Some of the reasons for HOT prescriptions
A Review of Literature
A systematic search of the literature was carried out on medical and pharmaceutical databases. The databases used were as follows: Embase (1980-28.2.2016), International Pharmaceutical Abstracts (1970-28.2.2016), PubMed (1950-28.2.2016), Web of Science (1900-28.2.2016) and Cochrane Library (1970-28.2.2016). Where possible, MeSH and EMTREE were used within the PubMed and Embase databases. The search strategy involved using related variants of the search words, which were combined in the search field using the Boolean operator “OR”. Also, the Boolean operator “AND” was used to put together some of the keywords used in the systematic literature search. An inclusion and exclusion criteria were developed and used to screen the titles and abstracts of articles for admissibility. The strategy used in the research process, the citations, and the resulting hits are shown in Table 1 below.
|
Table 1: The strategy used to search the literature |
|||||
|
Database |
The strategy used to search |
Retrieved citations 28-02-2016 |
Studies retrieved after the screening of title and abstract and eliminating duplicated articles |
||
|
Pub med |
("Adverse effects/Oxygen Inhalation Therapy" OR "mortality/Oxygen Inhalation Therapy")) OR advantage or ("Risk" OR "Risk Assessment")) OR "Patient Amenability") OR "Patient Satisfaction"[Mesh]) OR "Perception"[Mesh]) OR ( "Patient Outcome Assessment" OR "Treatment Outcome")) OR "Quality of Life")) AND Oxygen Inhalation Therapy [MeSH Terms]) AND (home OR long term OR nonstop oxygen therapy) |
1042 |
24 |
||
|
EMBASE
|
(Home oxygen therapy OR continuing oxygen therapy OR uninterrupted oxygen therapy) AND (Unfavorable drug reaction OR Mortality OR Benefit OR risk assessment or risk OR patient observance OR Patient satisfaction Perception OR Assessment of outcome OR Outcome treatment/OR quality of life
|
803 |
4
|
||
|
International Pharmaceutical Abstract (IPA)
|
(death or value or assessment of risk or risk or compliance of patients or perception or quality of life or assessment of outcomes or treatment assessment or satisfaction or unfavorable drug reaction or side effect)
AND oxygen therapy AND (home OR long-lasting OR uninterrupted oxygen therapy) |
19
|
1 |
||
|
Cochrane library |
Home oxygen therapy Long-lasting oxygen therapy ongoing oxygen therapy |
14
78 |
0
0 |
||
|
Web of science |
(death or value or assessment of risk or risk or compliance of patients or perception or quality of life or assessment outcomes or treatment assessment or satisfaction or unfavorable drug reaction or side effect) AND (oxygen therapy) AND (home or long-lasting or uninterrupted oxygen therapy) |
166 |
4 |
||
The criteria used to include and exclude studies
Studies included in the systematic review were those featuring adult recipients on oxygen therapy. The criteria used to include and exclude studies is as shown in table 2 below.
|
Table 2: Inclusion and Exclusion Criteria |
||
|
|
Inclusion |
Exclusion |
|
Population |
Adult individuals receiving home oxygen therapy for any related disease. |
Patients less than 18 years of age. |
|
Intervention |
Long term oxygen therapy; oxygen therapy delivered at home |
Patients who are either acute or in a hospital. |
|
Outcomes |
Articles featuring benefits, such as the quality of life, reduced rate of hospitalization and increased survival rates. Articles on risk, adherence, as well as satisfaction and perception. |
Articles listing all other outcomes apart from those highlighted in the inclusion criteria. |
|
Format |
Articles available in full text and the English language. |
All articles classified as conference abstracts, systematic reviews, letters, and case studies. All articles published in other languages apart from English. |
Literature search yield
The search process yielded a total of 2122 citations, but 2089 were excluded after the titles and the abstracts were checked against a criterion used to include and exclude studies. 33 articles had the full text available, among which 28 fitted the criteria used for inclusion and were incorporated into the current study. The process used to find and select the articles is summarized in figure 2.
Literature Analysis
The articles resulting from the search were grouped into four based on their area of focus – benefit, risk, adherence, and satisfaction, and perception. 28 studies were included in the systematic review. Among these, eight had been carried out in the UK – Janssens et al. (1997), Clark et al (2015), MRC (1981), Okubadejo et al (1996), Restrick et al (1993), Cornford (2000), Peckham et al (1998), and Goldbart et al. (2013) [4, 7-13]. The systematic review also had six studies carried out in the United States of America – Chang et al (2001), Muehlberger et al (1998), Robb et al (2003), Edelman et al (2008), Sharma et al (2015), and Assimacopoulos et al (2016) [14-19]. Two studies were carried out in Italy – Neri et al. (2006) and Rizzi et al. (2009) – while two others were carried out in Turkey – Demirel et al (2003) and Atiş et al (2001) [20-23]. The rest of the studies were either from Canada [24], Switzerland [7], East Asia [25], Poland [26], Denmark [27], Austria [28], France [29], Greece [30], New Zealand [31], and Australia [32]. Table 3 below illustrates the number as well as the groups of studies retrieved during the literature search.
|
Table 3: Number and groups of studies obtained from the literature search |
|
|
Focus |
Number of the group of studies found |
|
Benefit |
3 RCT studies – Górecka (1997), MRC (1981), and Clark et al (2015).
4 Observational prospective studies – Eaton et al (2004), Rizzi et al (2009), Okubadejo et al (1996), and Janssens et al (1997).
1 retrospective study – Cho et al (2015). |
|
Risk |
8 Retrospective studies – Robb et al (2003), Chang et al (2001), Muehlberger et al (1998), Murabit & Tredget (2012), Litt et al (2012), Assimacopoulos et al (2016), Sharma et al (2015), and Edelman et al (2008).
1 Observational prospect study – Edelman et al (2008). |
|
Adherence |
8 Observational prospective studies – Ringbaek et al (1999), Atiş et al (2001), Peckham et al (1998), Katsenos et al (2004), Restrick et al (1993), Pepin et al (1996), Neri et al (2006), and Demirel et al (2003). |
|
Satisfaction and Perception |
3 Observational prospective qualitative studies – Wilson et al (2006), Cornford (2000), and Goldbart et al (2013). |
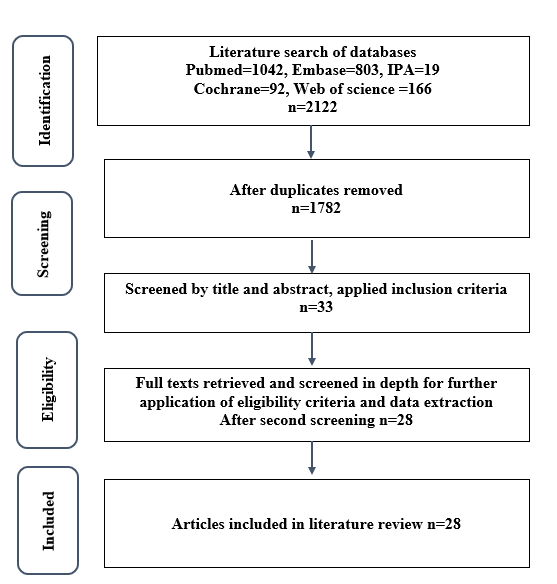
Figure 2. Flow chart illustrating the process used to find and select the articles.
Benefits of HOT
Benefits associated with HOT may include the decrease of either the death rate from all causes of death, the possibility of hospitalization, or advancement in the value of life.
Reduction of the survival-rate from all causes of death
HOT has differing indications. As such, proof of the benefits of survival among patients receiving HOT ranges from those with benign to mild, or acute hypoxemia.
- Acute Hypoxaemia
The Medical Research Council Working Group carried out a randomized controlled trial of HOT in the UK across various centers. The study was carried out on three sites and involved a total of 87 patients diagnosed with COPD as well as acute hypoxemia. The researchers assigned the patients into two indiscriminately matched groups – the HOT and non-HOT groups. Patients classified in the HOT unit utilized oxygen for 15 hours each day, while the non-HOT group acted as a control. The researchers compared the baseline characteristics of each group. Among the participants in the study were smokers and those on drug therapy. Within the three studies, adherence was tested differently. In essence, adherence was tested by either noting down the amount of time used on oxygen, carrying out arbitrary visits, or assessing the cylinders. A follow-up of five years was carried out, in which 19 out of the 42 patients in the HOT grouping, and 30 out of the 45 in the non-HOT grouping regrettably died (a P-value was not given in the study). Lesser risk of death (5.7%) was more common among the females in the HOT grouping as matched to those in the non-HOT grouping (36.5%, P<0.05). The authors were only able to test the difference in mortality between the male groups after 500 days. The difference was 12% for HOT and 29% for the non-HOT group (P=0.04). On the overall, the patients classified in the HOT class reported a reduced rate of mortality. Even so, this group was only able to report survival benefits after 1 year and 135 days of being on oxygen treatment. It was also clear from the findings that HOT either decelerated or impeded deterioration among the patients who endured their condition [4].
Minor to Modest Hypoxemia
A multicenter RCT was conducted by Górecka et al. (1997) in Poland. The goal of the research was to liken the impact of LTOT to that of no LTOT on the endurance of 135 patients diagnosed with COPD and modest hypoxemia. Unlike the MRC study, Górecka et al. (1997) did not include a sample of smokers. The median age of the study participants was 61, and 29% of them were undergoing steroid treatment. The authors used a meter reading to keep an eye on the observance of LTOT. The outcome of a follow-up carried out in three years showed no significant differences in the existence of the LTOT grouping (55.9%) compared to the non-LTOT grouping (47.8%), (P=0.89). Based on these observations, it is was evident that LTOT administered to COPD patients with mild hypoxemia did not result in any significant survival benefits.
Risk of hospitalizations
Cho et al (2015) carried out a large retrospective study investigating the correlation between HOT and the rate of hospitalization among COPD patients in East Asia. A follow-up was carried out in the study for 7 years. The authors categorized the patients on HOT into four classes based on their respiratory impairment. Grade 1 had FEV1 not more than or equivalent to 25% or PaO2 not more than or equivalent to 55 mm Hg. Grade 2 had FEV1 that was less than or equal to 30% or PaO2 that was between 56 and 60 mm Hg. Grade 3 had FEV1 that was less than or equal to 40% or PaO2 that was between 61 and 65 mm Hg. The three classes of patients were compared to the last class who were not participating in HOT sessions. The outcome of the study revealed a relative risk (RR) of hospitalization of 1.27 (95% CI 1.01-1.60) among the non-HOT group. A multivariate assessment of patients in grade one revealed that the RR for the group classified as not participating in the HOT sessions was 1.65 (95% CI 1.25 -2.18). Among the patients in the 2nd and 3rd grades, the outcome showed no statistically meaningful difference in the probability of hospitalization. The results also showed that HOT resulted in a 27% decrease in the risk of hospitalization among patients in the first group. These observations can be explained by the fact that hospital admission associated with exacerbation is more frequent among patients diagnosed with serious COPD. Based on the outcome of the research, the authors established the significance of using HOT among patients with PaO2 less than 55 mm Hg or those with a predicted FEV1 less than 25% to avert hospital admissions. This conclusion is significant considering that the MRC study did not verify this benefit of LTOT [4], despite being a randomized controlled trial.
There is proof of the benefits of HOT, but studies with low adherence have failed to make this benefit clear. In one follow-up study carried out in Italy for 10 years by Rizzi et al (2009), the authors focused on two analogous cohort groups consisting of either home care (HC) or standard care (SC). The researchers examined the impact of following up patients on home care on episodes of exacerbation, mortality, and admission rates at the hospital. The outcome of the home care group was compared to that of the standard care group. The outcome showed that the rate of survival was statistically meaningful between the home care and the standard care groupings, with this outcome benefiting the home care group more (P=0.0001). Moreover, the home care group reported reduced exacerbation rates compared to the standard care group. Based on the outcome of the study, it was evident that HC was useful in bringing down the rates of hospital admission and death among patients diagnosed with COPD and benefiting from HOT.
Quality of life
Quality of life is the general well-being of individuals and communities, outlining negative and positive aspects of life [33, 34]. There is no fascinating proof that LTOT is valuable to Health-Related Quality of Life (HRQOL). From the current scholarly work, it was evident that HRQOL went up or at least did not go down. Among studies that used the St. George’s Respiratory Questionnaire (SGRQ), an outstanding score suggested poor HRQOL. The SGRQ score was largely dependent on activity, symptoms, as well as effects. Alternatively, studies used the Chronic Respiratory Questionnaire (CRQ), whereby an outstanding score showed good HRQOL. CRQ scores were largely based on fatigue, dyspnea, mastery, as well as emotional function. Apart from these, many other measurements have been identified in the literature.
- Chronic Respiratory Questionnaire
A prospective study by Eaton et al (2004) used a sample of 68 patients diagnosed with COPD. The study sample was from New Zealand and had been referred to as an oxygen service to evaluate fluctuations in HRQOL within a follow-up period of six months. The authors likened 43 patients on LTOT to 25 who were not on LTOT. The study excluded patients who were either smokers or those diagnosed with primary comorbidities. Study participants in the LTOT grouping utilized oxygen for an average of 14.6 hours each day based on readings obtained from a meter. Baseline CRQ was used to measure HRQOL. Additional measurements were taken at 2 and 6 months. The outcome of the study showed that LTOT patients experienced meaningful advancements in HRQOL that were statistically significant at periods of 2 and 6 months. At 2 months, the average overall CRQ score was 8.10 for the LTOT grouping (95% CI, 3.02-13.17). Measurements are taken at 6 months also showed an average total score of CRQ of 9.26 (95% CI, 2.37-16.15). Contrariwise, HRQOL in the group that was not on LTOT reported a decline throughout the study. Another prospective study within this domain was completed by Crockett et al (1999). The study was completed in Australia to examine the impact of HOT on HRQOL. The study sample consisted of 114 patients who were on LTOT, among which 59 were male and 55 were female. The authors measured CRQ scores at 3, 6, and 12 months. Unlike Eaton et al (2004), Crockett et al (1999) did exclude for comorbidities. The study sample used LTOT for a mean period of 19 hours every day. The outcome of the study showed key improvements in fatigue among the male sample at 3, 6, and 12 months. Emotional function and mastery improved, even though the changes were not meaningful from a statistical perspective. The findings also showed a statistically significant upturn in mastery among the female participants at three, six, and twelve months. There was also a substantial positive change in fatigue and emotional function at 3 and 6 months. Nonetheless, the positive changes in emotional function and fatigue were not statistically meaningful based on measurements taken at 12 months. The decrease in the sample size may account for these findings. In general, male, and female samples on LTOT stated statistically weighty changes in HRQOL in a positive direction. Females recounted considerable changes in HRQOL (statistically significant), while the outcome from the male sample was less compelling. A possible reason for this is the increased identification of gender differences while responding to questions on the smoking of cigarettes.
- St. George’s Respiratory Questionnaire
One study by Janssens et al (1997) used a sample of home patients from Switzerland to carry out descriptive research. The focus of the study was to define the HRQOL changes happening in 79 patients within 1 year. The changes were measured using SGRQ. After 1 year, the researchers reported that the survival rate of the sample was 69%. The researchers found low median HRQOL index scores since 55% of the patients had scored less than 50 out of 100. Based on these findings, the authors recommended that healthcare providers should provide suitable support to HOT patients to make the HRQOL score much better. Another study by Okubadejo et al (1996) was carried out in the United Kingdom to examine the impact of HOT on HRQOL. The authors used SGRQ to measure the impact on 19 COPD patients on LTOT. The control in the study was 18 non-LTOT patients diagnosed with COPD. The researchers followed the study sample for six months. The LTOT group used an average of 16.7 hours each day. SGRQ measurements were taken at 2 weeks, 3 months, and 6 months. The findings showed a poor quality of life considering that the LTOT group reported above-average SGRQ total scores compared to the group that was not on LTOT. The scores were statistically significant. Measurements taken at 2 weeks showed no significant changes from the baseline SGRQ scores between the group of patients on LTOT and those not on LTOT (6.8 ± 12.7; 4 ± 10.7) in that order (P=0.48). measurements taken at 6 months showed no major differences in the change in HRQOL from baseline between the LTOT and the group that was not on LTOT (1.3, SD 14.5, 2.9, SD 13.4), in that order (P=0.38). Despite the disparities in the changes of the SGRQ score between the LTOT and the group that was not on LTOT being non-significant, the findings showed that the LTOT did not undesirably have an impact HRQOL.
- Additional HRQOL measurements
A study by Clark et al (2015) carried out a randomized controlled trial at various centers in the United Kingdom. The goal of the research was to investigate the impact of HOT on HRQOL among patients diagnosed with severe symptomatic heart failure. The authors measured HRQOL with the help of the Minnesota Living with Heart Failure (MLwHF) questionnaire. The measurements were taken at 6 months. The outcome of the study showed that the disparity in the measurements was not statistically meaningful. Based on these findings of the measurements taken at 6 months, the authors concluded that there was no difference in the scores of the MLwHF questionnaires between the HOT group and the group that was not on HOT. The adjusted mean difference was -0.10 (95%CI-6.88 to 6.69; P=0.98). The outcome of the scholarly work suggested that HOT did not cause a reduction in HRQOL among patients diagnosed with heart failure. Besides, HOT did not seem to have a valuable influence on HRQOL. It is, however, necessary to acknowledge that the patients in the study reported a poor rate of adherence, considering that only 11% used the oxygen as was recommended. Also, the researchers resorted to choosing a control group consisting of patients with less brutal hypoxemia since it is immoral to suppress the supply of oxygen to patients diagnosed with acute hypoxemia. These two reasons may account for the findings that were not statistically significant (Clark et al 2015).
Risks of home HOT
The risk of HOT was demonstrated in 8 studies included in this review. Based on these studies, the risk is classified as a burn resulting from a patient benefiting from HOT. Table 4 shows a rundown of the results obtained on burns associated with HOT.
Chang et al (2001) carried out a retrospective study of patient records. The outcome of the review illustrated that out of the 1,335 cases associated with burns, 23 cases were linked to HOT. Among the 23, 2 resulted in death over 12 years. There was a low percentage (1.7%) of burn cases associated with HOT. What is striking, however, is the increase in the occurrence of the cases. As Chang et al (2001) observed, 11 patients represented in the initial 10 years of the research, while the remaining 12 represented during the final two years of the research. These findings can be supported by the upsurge in HOT use, together with factors associated with a population that was growing old. What’s more, most of the patients with burns resulting from HOT were identified in the in-patient locales. Underreporting may account for these observations since most of these patients may be treated as an outpatient as well.
Another retrospective review by Robb et al (2003) incorporated patients who had been treated as either in-patient or out-patient at a burn center for 10 years. The outcome of the study included 27 burn cases that were all linked to HOT. 15% (4) of these cases resulted in death. The most popular cause of the burns (89%) was smoking a cigarette while on oxygen therapy. The study by Robb et al (2003) makes important additions to scholarly work by demonstrating the significance of smoking cessation once a patient is placed on HOT.
Murabit and Tredget (2012) described the frequency of cases associated with burns among patients on HOT and smoking at the same time. The study was carried out for 9 years. The outcome of the research showed that 17 patients developed injuries that were less associated with smoking, and 11.8% of the patients succumbed to death at the time of hospitalization. Most of the patients stayed in the hospital for a mean duration of 42.8 ± 12.5 days. The mean days in the hospital were 15.2 days, which was high when equated to the overall burn injuries reported within the same hospital (1.7 days). Such a difference was not accounted for in the study by Chang et al (2001) and Robb et al (2003). Upon recovery, it was also clear from the study findings that 35% of the patients could not live on their own and needed placement in facilities designed for supportive living. Based on the findings, the study implied that the deterrence of such injuries promoted the safety of patients and facilitated their allocation of health-care resources.
Litt et al (2012) compared the age and average length of stay in their research to that of past scholarly works. The sample used by Litt et al (2012) was majorly made up of female participants (83.3%). The total body surface area (TBSA) of the participants was considered to be extreme at 17%. A possible explanation for this is that many of the patients with burns in past studies were categorized as an outpatient. Also, 66.7% of the patients suffered injuries that were hardly associated with smoking. Based on these observations, the authors determined that the follow-up and re-evaluation of patients could minimize the danger of burns linked with HOT. Another retrospective research by Muehlberger et al (1998) examined 21 patients for 7 years. The authors were interested in burn injuries developing hardly as a result of smoking while on HOT. Among the study participants, 17 patients reported having second-degree burns, 4 suffered full-thickness burns, while 2 patients needed debridement and grafting of the skin. In their findings, the researchers focused on the significance of education and cautioned the patients, their families, as well as the caregivers concerning the effects of smoking while on HOT. The findings also revealed that cannula tubes with a lesser amount of flammable substance can be used to prevent injuries from burns.
Sharma et al (2015) carried out two different study designs across 9 geographic regions. The outcome of the nested case-control design showed that patients with burns were two times likely to be on HOT than those without burns based on statistics collected for three months (OR, 2.43; 95% CI, 1.57-3.78). The other study, retrospective in nature, was done for a longer time of 22 months and revealed an absolute risk of burns of 2.98 per 1000 patients for study participants on HOT, and 1.69 per 100 patients for those not on HOT. The danger of burns related to HOT was determined to be 0.704 for every 1000 patients for each year, with the quantity required to cause damage being determined as 1421. The authors used a multivariable assessment to determine the elements related to burns among patients on HOT, which comprised of the presence of at least three comorbidities, male sex, as well as low socioeconomic status. The findings revealed that patients who had to burn injuries while on HOT had a rate of mortality that was 10 times more than those patients who did not have burn injuries. Sharma et al (2015) also pointed out the significance of educating patients and providing them with counseling on the risks of burns allied to HOT. In another prospective study, Edelman et al (2008) noted that 14 patients developed injuries from smoking burns, which were developed while on HOT over 2 years. The authors also noted that 1 of the patients died while at the emergency department, 1 was released from the ED, and 12 ended up being admitted to the hospital. Among the 12 who were admitted to the hospital, 50% regrettably died. Based on these findings, the authors recommended that patients undertaking HOT should stop smoking before commencing HOT. Another extensive retrospective review by Assimacopoulos et al (2016) tried to ascertain the occurrence of burn injuries associated with HOT during 10 years. The study findings revealed that burns associated with HOT increased substantially from below 50 cases each year to about 200 cases annually. The increase was equivalent to 14% (P<0.001). One surprising observation from the study was that 83% of the burns reported were related to smoking. Based on these findings, the researchers emphasized the significance of quitting smoking and recommended that this should be a mandatory requirement for all the patients being put on HOT.
|
Table 4: Summary of papers found evaluating HOT related burns |
||||||||
|
Study design |
Retrospective |
Prospective |
||||||
|
Authors |
Change |
Robb |
Murabit |
Litt |
Muehlberger |
Sharma |
Assimacopoulos |
Edelman |
|
Years |
1986-98 |
1992-2001 |
1999-2008 |
2007-12 |
1990-97 |
2001-10 |
2002-11 |
2004-05 |
|
Details of the patients |
||||||||
|
The number of patients |
23 |
27* |
17 |
6 |
21 |
279 |
957 |
14** |
|
The average age (years) |
70 |
68.1 |
69.1 |
72 |
60.4 |
72.26 |
63.9 |
66 |
|
Percentage of male patients |
30 |
51.9 |
52.9 |
16.7 |
76.2 |
50.8 |
60 |
71 |
|
Percentage of those with COPD |
87 |
93 |
100 |
100 |
90.5 |
100 |
NA |
100 |
|
Details on the admission |
||||||||
|
Average duration of stay (days) |
NA |
4.4 |
42.8 |
22.5 |
3.6 |
NA |
7.2 |
22 |
|
Average TBSA% |
3.9 |
8.4 |
2.8 |
17 |
2 |
NA |
4.2 |
3.9 |
|
Outcome |
||||||||
|
Mortality % |
8.7 |
15 |
11.8 |
16.7 |
0 |
4.82 |
9 |
50 |
|
* Only 13 of the patients were admitted, while only 14 were attended to as out-patient. ** 12 patients were taken in and attended to as in-patient. |
||||||||
Adherence to HOT
Adherence to HOT was examined in 8 studies which defined devotion to oxygen therapy using the registered day to day use of oxygen (measured in hours). The measurements were either through the self-reports of the patients, objective assessments or through both avenues. Table 5 provides a brief overview of the evidence obtained from the studies on adherence to HOT.
- Adherence to the right time of oxygen (objective assessments as well as self-reports from the patients)
Atiş et al. (2001) focused on the self-reports of Turkish patients on their adherence to HOT. The researchers sent a questionnaire to 1100 patients and achieved a 34.5% response rate. Atiş and colleagues were aware that most patients tend to misjudge the amount of oxygen used. As a result, they also measured the track record of the concentrator after 3 months to make an objective assessment. The outcome of the study revealed an average oxygen concentrator of 9 ± 6.8 hours per day. Besides, 87% of the study participants were also established to have COPD. The study estimated self-reported observance to be 28.8% and the real observance to be 21.3% based on measurements done through a machine clock counter. There was a significant disparity between the reports provided by the patients and the computed adherence (P=0.03). When measurements were taken to cover for age, sex, social status, and the level of education, the authors found no statistical variation between the patients who complied and those who were not. A key observation, however, was that most of the non-compliant patients tended to smoke regularly than the conforming ones (P<0.01). Training associated with oxygen treatment was also provided on a less regular schedule (P<0.001). The findings also revealed that follow up procedures were done less frequently (P=0.002). According to the study findings, 34.5% of the patients suggested that their physicians checked upon them regularly. The rate of compliance increase 3.8 times as a result of close follow-up, thereby illustrating the possibility that early education and close follow up procedures can increase the rates of compliance among patients receiving HOT. Another study by Ringbaek et al (1999) evaluated compliance rates among 125 patients in LTOT. The findings showed that 65% of the study participants utilized oxygen for 15 or more hours every day. However, the findings also showed that 13% of the patients used oxygen for a period of fewer than 15 hours each day, and 29% of the study participants used oxygen for fewer than 15 hours every day. Research by Katsenos et al (2004) evaluated the rate of observance among patients on HOT and identified related elements. The study sample was made up of 249 patients, who responded to a questionnaire. The investigation team also evaluated the participants by visiting their homes. 74.7% of the study participants had COPD. The outcome of the study was surprising considering that more than 50% of the study participants suggested that they had not gotten inscribed instructions concerning the use of HOT. Additionally, 63% of the sample did not recognize the significance of HOT in the treatment of their illnesses. The average time of oxygen use was 9.7 ± 6.09, which is equivalent to that reported in the study by Atiş et al (2001). Patients who followed HOT consisted of only 26.9% of the sample size. The research also showed that there was no statistical difference in the ability to follow HOT between those who smoked and those who did not (P=0.88). From the findings of the study, it was clear that implementing a home-care program was necessary for ensuring the compliance of patients with HOT. Restrick et al (1993) carried out research consisting of 180 patients, whose data was collected from three health services in London. A structured questionnaire was used to interview the study sample. The interviews were carried out through home visits. 84% of the study sample were diagnosed with COPD. The average time prescribed was 15 hours. 74% of the study sample suggested that they used oxygen for a period of 12 or more hours. Since compliance with HOT was outstanding, the study suggested that patient compliance and the best possible treatment can be achieved by organizing home visits. Another research study by Peckham et al (1998) examined the benefits of evaluation and learning on the rate of adherence. The authors hypothesized that assessment and education could increase the effectiveness of HOT. The study sample was obtained from the UK and was divided into two. The first group, consisting of 45 patients, took part in an evaluation and education program designed for HOT. The second group, featuring 41 patients, did not receive any formal training before a HOT prescription. 82% of the study participants who received training and assessment managed to use their oxygen for 15 or more hours, while only 18% of the control group were able to do this (P=0.0002). Additionally, 93% of the patients who were trained and assessed were informed about the advantages of HOT. About 41% of the patients in the control group clearly understood the reasons for being on HOT (P=0.00001). Based on the findings of this study, it was evident that patients who were trained on HOT clearly understood the justifications for the benefits of oxygen and had a superior rate of adherence to this form of treatment. It is, therefore, clear from these findings that education impacts the understanding and perceptions of a patient concerning oxygen treatment.
- Adherence to the right time of oxygen (self-reports from patients)
Neri et al (2006) examined the behavior and understanding of HOT among patients. The authors carried out an observational study consisting of 1,504 patients distributed across multiple centers. All the outpatients who had been on HOT for a minimum period of 6 months completed a survey. The findings showed that 6.5% of the patients smoked while on HOT and 21% of the study sample used oxygen for fewer than 15 hours every day. Key times when the patients used oxygen for fewer hours than recommended were as follows – daytime (P=0.02), night time (P=0.0036), as well as during workout (P=0.002). A majority of the study participants experienced improvements after HOT, while 12% did not experience any improvements based on their self-reports. An interesting observation from the study was that those patients who reported no improvements used oxygen for fewer hours than recommended. These findings imply that awareness programs must be developed to provide patients with valuable information concerning the use of portable oxygen treatment. Taking such an approach could help enhance HOT practice.
- Adherence to the prescribed time of oxygen (objective assessment)
Prospective research by Demirel et al (2003) evaluated the compliance of 127 patients to HOT. The investigators visited each patient in the study to ascertain the use of oxygen. The findings revealed that 43.3% of the study participants used oxygen therapy for 15 or more hours. Only 11% of the study sample used oxygen for at least 12 hours or more.
Pepin et al (1996) used a study sample of 903 patients to determine the degree of compliance to LTOT. The study was carried out at different centers to identify the factors affecting compliance among patients. The authors calculated compliance by comparing the day to day utilization of LTOT to the day to day specified time of LTOT. 45% of the study sample used HOT for 15 or more hours each day. A major setback in the study was the fact that data on the day to day recommended oxygen was only available for 564 patients. Among these patients, 89% were expected to receive oxygen for more than 12 hours, while 87% were required to receive oxygen for 15 or more hours each day.
|
Table 5: Summary of proof on the adherence to HOT |
|||
|
Author/year |
Study population (n) |
Self-reported (SR) or objective measure (OM) |
Adherence rate percent |
|
Atiş et al 2001 |
379 |
SR
OM |
28.2% stated that they used oxygen for 15hours each day 21.3% used oxygen for 15 hours every day |
|
Ringbaek et al 1999 |
125 |
SR
OM |
87% stated that they used oxygen for 15 hours every day 65% used oxygen for 15 hours each day |
|
Restrick et al |
176 |
SR
OM |
28% stated that they did not wear the cannula for two hours 74% used the cannula for 12 hrs per day |
|
Katsenos et al 2004 |
249
|
SR
OM |
No self-reports were identified.
26.9% used oxygen for 15 hours each day. |
|
Neri et al 2006 |
1504 |
SR |
85% stated that they used oxygen for 15 or more hours each day |
|
*Peckham et al 1998 |
45
41 |
OM
OM |
82% used oxygen for 15 hours or more each day 44% used oxygen for 15 hours each day |
|
Demirel et al 2003 |
n=127 |
OM |
43.3% used oxygen for 15 hours each day 11% used oxygen for more than 12 hours every day |
|
Pepin et al 1996 |
n=903 |
OM |
45% used oxygen for 15 hours each day |
|
* The research matched the differences between the two groups. One of the groups benefited from early assessment training while the other group benefitted from early assessment as well as training. |
|||
Perception and satisfaction of HOT
There are quite a few studies that openly deal with the views of the patients on oxygen therapy. Generally, three published studies had explored the views of the patients on HOT, two of the studies being from the UK. From these studies, the perceptions of the patients were considered to be diverse. In one qualitative study, Cornford (2002) examined the perceptions of the patients concerning HOT. The authors used semi-structured interviews to obtain the opinion of 24 patients in their homes. The research findings revealed two different approaches to the use of home oxygen. However, the findings also revealed that oxygen treatment assisted the patients to establish the ability to control their health issues. Being dependent was a primary concern in the study, even though not all patients were affected by this concern. Some patients did not worry much about dependency after realizing that they could not stay alive without oxygen. The study findings, however, illustrated the benefits of discussing the perceptions of the patients concerning HOT to provide both comfort and assistance to these patients. In the same manner, another study by Goldbart et al (2013) used focus group interviews on a sample of 19 patients. Based on the study findings, dyspnea helped most patients to feel safe and improve their social activity. Even so, a few patients described oxygen treatment as being restricting. In their conclusion, the authors suggested that it was important to provide patients with better information on public health. A qualitative study by Wilson et al (2006) used a sample of 17 patients [35]. The findings of the study identified embarrassment as being common, an issue that is also raised in the research by Neri et al (2006). About 41% of the patients used oxygen outside their house due to the shame associated with this approach. Wilson et al (2006) also noted the description of oxygen therapy as a milestone in the path of disease and as a symbol of deteriorating health [35].
Discussion and limitations
Benefits of HOT
The review has reported proof of the advantages of HOT based on the survival of patients diagnosed with COPD. It is clear from this study that HOT increased the rate of survival among COPD patients diagnosed with mild to moderate and acute hypoxemia. However, some of the findings in this review are quite conflicting. The conflict arises from the fairly small sample size (n=87), the lack of comorbidities, and the young age of study participants (below 60 years) [4]. These conditions raise questions concerning the generalization of the study findings, especially among older patients. The lack of survival benefit among mild to moderate hypoxaemic patients can be attributed to the impact of steroid therapy, considering that 29% of the study participants were on steroid therapy [26]. This is conflicting considering that study participants in Rizzi et al (2009) were on steroid therapy but still showed survival benefits. From these findings, it is clear that the concept of survival is not appropriate or viable to measure and requires many study participants. In another study by Górecka (1997), study participants used oxygen for 13.5 hours each day, even though a minimum of 15 hours were needed each day to report survival benefits among less acute hypoxaemic patients. Proof of this is evident in the study by Rizzi et al (2009) where moderate hypoxaemic patients showed survival benefits after using oxygen for 22 hours each day. Considering that it is disreputable to carry out RCTs among hypoxaemic patients, conclusions should be obtained from the partial evidence available which seems to support the survival benefits among these patients. Concerning HRQOL, several approaches were used in the identified studies. Eaton et al (2004) and Crockett et al (1999) used CRQ; Janssens et al (1997) and Okubadejo et al (1996) used SQRC, and Clark et al (2015) used MLwHF. However, the findings from these studies were unconvincing considering that different measures were used. There is a need for additional research to clarify these outcomes. It is also necessary to consider the shortcomings of the reviewed studies. In essence, the studies presented a small sample size that ranged from 41 to 217 in all the studies except in Cho et al (2015) and Rizzi et al (2009). The small sample size together with the unsatisfactory adherence to LTOT in the studies by Clark et al (2015) and Górecka (1997) implies that patients may not experience the full clinical benefits even with continuous use of oxygen. These factors may have influenced the non-significant differences in some of the outcomes. It is also important to recognize gender differences, their relation to cigarette smoking, and the impact these factors may have towards no benefits [9, 32]. Hence, there is a need for an RCT of LTOT stratified for smoking, even though such a study is less likely to happen. Nonetheless, there are many reasons to make certain that patients follow the recommended guidelines for LTOT; ensure the treatment of reversible factors, and promote a priority end to smoking.
Risks of HOT
The literature revealed that the use of oxygen at home is associated with certain risks, such as serious burns. In all the studies included in this review, the most popular reason for burns was smoking while on HOT. Muehlberger et al (1998) and Murabit and Tredget (2012) identified that smoking while on HOT was the primary reason for burns in all the examined cases. The actual number of burn cases is also underestimated since most of the literature focuses on patients receiving treatment at burn centers [14, 15, 19, 24, 28]. Some studies also captured inpatient and individuals who had been treated as either outpatient or in the emergency department [16-18]. The studies also revealed a doubling of the mean number of burns associated with HOT [14, 19, 24, 28]. Many researchers also noted a rise in the occurrence of burns related to HOT sessions, which can be explained by the increase in the number of HOT users. These observations imply that healthcare professionals need to notify patients of the consequences of smoking while on HOT. These burn injuries can, however, best be eliminated by encouraging smoking cessation and increased assessment of patients and those living next to them before initiating the use of oxygen at home. A feasible conclusion from this is that patients and caregivers need to be educated about the risks to save lives and minimize injuries.
Adherence to HOT
The outcome of 8 studies revealed that the rate of adherence to oxygen therapy ranged between 21 and 85%. These rates of adherence were necessary for attaining the required minimum duration of 15 hours each day. Atiş et al (2001) and Pepin et al (1996) suggested that low adherence arose from the lack of education on the use of oxygen. Atiş et al (2001) also proved that regular follow up procedures resulted in an outstanding rate of adherence. Atiş et al (2001) and Katsenos et al (2004) also demonstrated that non-smoking and low PaO2 resulted in good compliance. On the contrary, Atiş et al (2001), Restrick et al (1993), Katsenos et al (2004), and Ringbaek et al (1999) showed little concern over the impact of age and sex on the rate of adherence to HOT. Hence, it is problematic to draw strong conclusions on the rate of adherence to HOT. The most objective approach used to measure adherence involves the use of a patient questionnaire or a clock included in the oxygen concentrator. These approaches are hindered by certain drawbacks. Atiş et al (2001) and Ringbaek et al (1999) note that some patients tend to miscalculate the quantity of oxygen used. What’s more, the oxygen used represents the extreme amount of oxygen used instead of the quantity that is being breathed by the patient. For instance, 27% of patients in one study suggested that they did not put on the cannulae even though the concentrator was on for 2 hours. That means that the number of hours of oxygen use reported by most patients exceeds the real number [10].
Perception and satisfaction of HOT
The study provides insight into the assessments of oxygen therapy among patients. Patients seem to doubt the goal and benefits of HOT. The outcome of most studies showed positive experiences among patients on HOT. Even so, the experiences of the patients differed and a few of them reported having negative perceptions. These contradictory outcomes suggest that it is difficult to estimate the effect of HOT on the lives of patients.
Conclusion
The literature review sought to examine the risks, benefits, adherence, as well as the perception of HOT among patients. A primary risk identified in this review is associated with HOT burns. In terms of the benefits of HOT, this study suggests the need for additional studies to provide more information and justify the positive outcomes. The study recommends initiating more studies focused on examining the benefits of HOT in regards to survival, HRQOL, as well as hospitalization. These studies may, however, be hindered by the inability to provide HOT to eligible patients. Studies on adherence, more so in the UK will be incredibly useful in the future since the literature review could only identify two studies from this locality. Still, improvements can be made to ensure adherence to HOT by all patients. Healthcare professionals should also consider providing regular follow-up to their patients. From this review, it is also clear that negative perceptions can result in poor education. On the overall, it is important to conduct more research to examine the perceptions of patients on HOT and factors contributing to those insights. Research in this direction will help promote the better clinical practice of HOT.
Acknowledgement
This research was funded by the Deanship of Scientific Research at Princess Nourah bint Abdulrahman University through the Fast-track Research Funding Program.
References
- Hanawi SA, Saat NZ, Zulkafly M, Hazlenah H, Taibukahn NH, Yoganathan D, Abdul Rahim NN, Mohd Bashid NA, Abdul Aziz FA, Low FJ. Impact of a Healthy Lifestyle on the Psychological Well-being of University Students. Int. J. Pharm. Res. Allied Sci. 2020 Apr 1;9(2):1-7
- Ahmadinejad M, Hashemian M, Noradini Z, Ahmadipour M. Evaluation the Effect of New Transdermal Oxygen Therapy Method on Healing of Pressure Ulcer in Children. Int. J. Pharm. Phytopharm. Res. 2020;10(1):61-
- Barach, A.L. The therapeutic use of oxygen, Journal of the American Medical Association, 1992; 79(9): 693-699.
- Medical Research Council Working Party. Long term domiciliary oxygen therapy in chronic hypoxic cor pulmonale complicating chronic bronchitis and emphysema: Report of the Medical Research Council Working Party, Lancet, 1981; 1(8222): 681-686.
- Nhsnetwork.Home Oxygen Service Assessment and Review Good Practice Guide 2011. www.pcss.nhs.uk
- Hardinge, M., Annandale, J., Bourne, S., Cooper, B., Evans, A., Freeman, D., Green, A., Hippolyte, S., Knowles, V., MacNee, W., McDonnell, L., Pye, K., Suntharalingam, J., Vora, V., Wilkinson, T. British Thoracic Society guidelines for home oxygen use in adults: accredited by NICE, Thorax, 2015; vol. 70, (Suppl 1): i1-i43.
- Janssens, J.P., Rochat, T., Frey, J.G., Dousse, N., Pichard, C., Tschopp, J.M. Health-related quality of life in patients under long-term oxygen therapy: a home-based descriptive study, Respiratory medicine, 1997; 91(10): 592-602.
- Clark, A.L., Johnson, M., Fairhurst, C., Torgerson, D., Cockayne, S., Rodgers, S., Griffin, S., Allgar, V., Jones, L., Nabb, S., Harvey, I. Does home oxygen therapy (HOT) in addition to standard care reduce disease severity and improve symptoms in people with chronic heart failure? A randomized trial of home oxygen therapy for patients with chronic heart failure, Health technology assessment (Winchester, England), 2015; 19(75):1-120.
- Okubadejo, A.A., Paul, E.A., Jones, P.W., Wedzicha, J.A. Does long-term oxygen therapy affect quality of life in patients with chronic obstructive pulmonary disease and severe hypoxemia? European Respiratory Journal, 1996; 9(11): 2335-233
- Restrick, L.J., Paul, E.A., Braid, G.M., Cullinan, P., Moore-Gillon, J., Wedzicha, J.A. Assessment and follow up of patients prescribed long term oxygen treatment, Thorax, 1993; 48(7): 708-713.
- Cornford, C.S. Lay beliefs of patients using domiciliary oxygen: a qualitative study from general practice, Br J Gen Pract, 2000; 50(459):791-793.
- Peckham, D.G., McGibbon, K., Tonkinson, J., Plimbley, G., Pantin, C. Improvement in patient compliance with long-term oxygen therapy following formal assessment with training, Respiratory medicine, 1998; 92(10): 1203-1206.
- Goldbart, J., Yohannes, A.M., Woolrych, R., Caton, S. ‘It is not going to change his life but it has picked him up’: a qualitative study of perspectives on long term oxygen therapy for people with chronic obstructive pulmonary disease, Health, and quality of life outcomes, 2013; 11(1): p.1.
- Chang, T.T., Lipinski, C.A., Sherman, H.F. A hazard of home oxygen therapy, Journal of Burn Care & Research, 2001; 22(1): 71-74.
- Muehlberger, T., Smith, M.A., Wong, L. Domiciliary oxygen and smoking: an explosive combination, Burns, 1998; 24(7): 658-660.
- Robb, B.W., Hungness, E.S., Hershko, D.D., Warden, G.D., Kagan, R.J. Home oxygen therapy: adjunct or risk factor? Journal of Burn Care & Research, 2003; 24(6): 403-406.
- Edelman, D.A., Maleyko-Jacobs, S., White, M.T., Lucas, C.E., Ledgerwood, A.M. Smoking and home oxygen therapy—a preventable public health hazard, Journal of burn care & research, 2008; 29(1): 119-122.
- Sharma, G., Meena, R., Goodwin, J.S., Zhang, W., Kuo, Y.F., Duarte, A.G. Burn injury associated with home oxygen use in patients with chronic obstructive pulmonary disease. In Mayo Clinic Proceedings 2015; 90(4): 492-499. Elsevier.
- Assimacopoulos, E.M., Liao, J., Heard, J.P., Kluesner, K.M., Wilson, J., Wibbenmeyer, L.A. The national incidence and resource utilization of burn injuries sustained while smoking on home oxygen therapy, Journal of Burn Care & Research, 2016; 37(1): 25-31.
- Neri, M., Melani, A.S., Miorelli, A.M., Zanchetta, D., Bertocco, E., Cinti, C., Canessa, P.A., Sestini, P. Educational Study Group of the Italian Association of Hospital Pulmonologists. Long-term oxygen therapy in chronic respiratory failure: a Multicenter Italian Study on Oxygen Therapy Adherence (MISOTA), Respiratory medicine, 2006; 100(5): 795-806.
- Rizzi, M., Grassi, M., Pecis, M., Andreoli, A., Taurino, A.E., Sergi, M., Fanfulla, F. A specific home care program improves the survival of patients with chronic obstructive pulmonary disease receiving long term oxygen therapy, Archives of physical medicine and rehabilitation, 2009; 90(3): 395-401.
- Demirel, H., Demir, T., Umut, S. Retrospective evaluation of patient compliance in continuous oxygen therapy, Respiration, 2003; 70(2): 149-153.
- Atiş, S., Tutluoğlu, B., Buğdayci, R. Characteristics and compliance of patients receiving long-term oxygen therapy (LTOT) in Turkey, Monaldi archives for chest disease, 2001; 56(2): 105-109.
- Murabit, A., Tredget, E. Review of Burn Injuries Secondary to Home Oxygen, Journal of Burn Care & Research, 2012; 33(2):212-217.
- Cho, K.H., Kim, Y.S., Nam, C.M., Kim, T.H., Kim, S.J., Han, K.T., Park, E.C. Home oxygen therapy reduces risk of hospitalization in patients with chronic obstructive pulmonary disease: a population-based retrospective cohort study, 2005–2012, BMJ open, 2015; 5(11): p.e009065
- Górecka, D., Gorzelak, K., Sliwiński, P., Tobiasz, M., Zieliński, J. Effect of long-term oxygen therapy on survival in patients with chronic obstructive pulmonary disease with moderate hypoxaemia, Thorax, 1997; 52(8): 674-679.
- Ringbaek, T., Lange, P., Viskum, K. Compliance with LTOT and consumption of mobile oxygen, Respiratory medicine, 1999; 93(5): 333-337
- Litt, E.J., Ziesche, R., Happak, W., Lumenta, D.B. Burning HOT: revisiting guidelines associated with home oxygen therapy, Int J Burns Trauma, 2012; 2(3): 167-70.
- Pepin, J.L., Barjhoux, C.E., Deschaux, C., Brambilla, C. Long-term oxygen therapy at home: compliance with medical prescription and effective use of therapy, CHEST Journal, 1996; 109(5): 1144-1150.
- Katsenos, S., Froudarakis, M.E., Charisis, A., Vassiliou, M.P., Constantopoulos, S.H. Long-term oxygen therapy in Ioannina, Respiration, 2004; 71(6): 619-624.
- Eaton, T., Lewis, C., Young, P., Kennedy, Y., Garrett, J.E., Kolbe, J. Long-term oxygen therapy improves health-related quality of life, Respiratory medicine, 2004; 98(4): 285-293.
- Crockett, A.J., Cranston, J.M., Moss, J.R., Alpers, J.H. Effects of long-term oxygen therapy on quality of life and survival in chronic airflow limitation, Monaldi Arch Chest Dis, 1999; 54(2): 193-196.
- Zahra NA. Low Back Pain, Disability and Quality of Life among Health Care Workers. Int. J. Pharm. Res. Allied Sci. 2020;9(2):34-44
- Marzangi A, Rezaei AS, Asl GR. Health literacy and its relation to quality of life in people with heart disease. Int. J. Pharm. Phytopharm. Res. 2018 Jun 1;8(3):25-32.
- Wilson, A., Crockett, A., Antic, R., Greville, H. A qualitative study of patient perceptions of home oxygen therapy, Primary Care Respiratory Journal, 2006, p.200.
Contact Meral
Meral Publications
www.meralpublisher.com
Davutpasa / Zeytinburnu 34087
Istanbul
Turkey
Email: [email protected]