Persistent limbal nodule in vernal keratoconjunctivitis that was improved with topical tacrolimus: A case report
Mitra Akbari
M.D. Assistant Professor of Ophthalmology, Cornea, and Anterior Segment fellowship, Eye Research Center, Eye Department, Amiralmomenin Hospital, School of Medicine, Guilan University of Medical Sciences, Rasht, Iran.
ABSTRACT
Purpose: To report our experience of managing a persistent limbal nodule associated with vernal keratoconjunctivitis (VKC) by topical tacrolimus eye drops. Methods: Case report. Results: A 9-year-old girl was referred to the hospital with the major complaints of photophobia and itching in eyes and foreign body sensation, redness, and ptosis in the left eye. She had a two-year history of gradually enlarging solitary limbal gelatinous mass on the nasal side of the limbus in a left eye, which according to the other signs and impression cytology (IC) was diagnosed as a VKC. This case highlights an isolated limbal nodule as an unusual presentation of vernal keratoconjunctivitis. As the disease in her left eye was more severe and persistent with maximum topical steroid usage, we started the topical tacrolimus (0.05%) eye drop, that a rapid therapeutic result was observed. After using the topical tacrolimus, all ocular surface inflammation and other symptoms rapidly disappeared and at 12-months follow-up, there was no recurrence of the limbal mass lesion and other symptoms and signs of VKC. Conclusion: The limbal mass like nodule may be the only obvious manifestation of VKC and should be considered in the differential diagnosis. In a refractory VKC, aqueous formulation of topical tacrolimus can be used and enhance remission in such complex cases and can resolve the patient’s complaints, rapidly.
Keywords: Limbal nodule, Vernal keratoconjunctivitis, Topical tacrolimus, Tacrolimus
Introduction
Vernal keratoconjunctivitis (VKC) is a seasonal bilateral chronic inflammatory allergic disease of the ocular surfaces, mainly occurring in adolescents and children living in dry and temperate regions. Tearing, mucoid discharge, photophobia, and itching are the main symptoms of VKC. Conjunctival hyperemia, superior limbal and tarsal papillae, and the involvement of cornea in the form of corneal neovascularization, plaque formation, shield ulcers, epithelial macroerosions, and punctate epithelial keratitis are also observed [1].
In patients with severe limbal VKC, chronic inflammation may result in a gradual loss of the function of corneal limbal stem cells, probably due to direct damage to the stem cells by toxic products of inflammatory cells such as eosinophils that infiltrate the limbus. The long duration and chronic nature of the disease are probably responsible for the affection of the secondary ocular surface that leads to clinical manifestations of limbal stem cell deficiency (LSCD) [2].
Corticosteroids still remain the main treatment for anterior segment inflammation and are the most commonly used topical anti-inflammatory drugs. However, unwanted ocular adverse effects such as cataract and glaucoma often preclude their use on a chronic basis. Calcineurin inhibitors such as tacrolimus and cyclosporine A are now commonly used as “steroid-sparing” topical agents to prevent and treat diseases with T-cell-mediated pathophysiology treatment of most ocular and corneal surface diseases [3, 4]. To prevent complications related to steroid, and in resistance cases, immunomodulatory agents such as topical tacrolimus and cyclosporine A are used to treat VKC. Tacrolimus is a drug that suppresses the immune system and has many applications in the ocular surface and corneal chronic inflammations [4, 5].
In this case report, we report a case of unusual presentation with a solitary limbal nodule and steroid-resistant VKC that properly managed with topical tacrolimus 0.05% eye drops.
Case Report
The patient was a 9-year-old girl with the complaint of decreased vision, ocular burning, and photophobia in both eyes since a few years ago that referred to our cornea clinic. Her complaints were aggravated since last year. Her past medical history was not remarkable. She was under medical treatment with topical steroids by several physicians but her complaints aggravated despite these medications. On slit-lamp biomicroscopy, bilateral cobblestone papillae, and a unilateral limbal nodule were observed in the left eye (Figure 1 A, B).
The differential diagnosis of the solitary limbal nodules may have many categories of allergic, inflammatory, neoplastic, and infectious diseases [6], but the presence of tarsal papillary hypertrophy led to the diagnosis of VKC. Our approach for confirming the diagnosis was impression cytology (IC). Impression cytology samples were taken from the cornea of the left eye and both upper eyelids tarsal conjunctiva.
Some goblet cells and many eosinophils could be seen on IC. According to this finding of IC, the diagnosis was the VKC with a hypertrophic limbal papillary reaction that presented as a solitary nodule and tarsal conjunctival papillary hypertrophy. The presence of some goblet cells in the IC was considered as some degree of stem cell damage in this case.
At all follow-up visits, findings were recorded using digital corneal photography (Imagenet; Topcon SL‐8Z, Tokyo, Japan). All benefits and risks were clearly explained and informed consent was obtained from the patient and her parents.
The patient had a history of a long-time treatment with mast cell stabilizers, topical antihistamines, and steroids that had not a marked improvement. This allergic inflammatory reaction was resistant to steroid therapy that was previously prescribed and we used for another 3 weeks without any improvement in her conditions. We used the tacrolimus eye drop by 0.05% every 6 hours that continued for one year. At that time, all symptoms and signs were reduced and the limbal nodule and tarsal conjunctival papillary hypertrophy were regressed. After 12 weeks along with decreasing ocular surface inflammation and shrinkage of limbal and tarsal papillary hypertrophy using topical tacrolimus (Figure 2 A, B), all symptoms and signs were completely resolved.
Tacrolimus eye drops preparation: These eye drops were reconstituted by the addition of a balanced salt solution to a tacrolimus vial (Prograf, Astellas Pharma Inc., Dublin, Ireland) under sterile conditions to reach a 0.05% concentration of tacrolimus. After the preparation, drops were stored at 4°C.
Discussion
Clinically, there are 3 forms of vernal keratoconjunctivitis: limbal, palpebral, and mixed. The palpebral form is characterized by flat-topped, polygonal, giant cobblestone papillae of the superior tarsal conjunctiva. The limbal form is less common and is characterized by a thickened, broad, opacification of the superior limbus. The tissue is composed of lymphocytes, plasma cells, macrophages, basophils, and a high level of eosinophils. The marked white Horner-Trantas dots are the epithelial and eosinophil debris. The cornea is involved in 50% of patients ranging from punctuate epithelial keratitis to superficial pannus to corneal shield (Togby’s) ulcers. Corneal ulcers are seen in 10% of cases. The VKC is clinically diagnosed based on the ocular examination as well as history. Conjunctival scrapings, exhibiting eosinophils may help to confirm, but are not essential for diagnosis [1, 2]. The bulbar form of conjunctivitis and enlargement of papillae give a poorer prognosis and lead to a higher rate of complication [7] as seen in our case.
Despite its name, VKC can frequently occur throughout the year. It has been proved that VKC is not only IgE-mediated, but it has a multifactorial pathogenesis, mediated by mast cells, IgE, eosinophils, Th2 lymphocytes, and a complex network of cell mediators and interleukins. In most cases, the clinical course of VKC is self-limiting and may be improved after puberty. Some VKC patients face vision-threatening complications usually due to corneal involvement and LSCD [1, 7] like our patient who had some goblet cells in the impression cytology.
For the treatment of VKC, various medications are used including antihistamines, anti-inflammatory non-steroidal medicines, and mast-cell stabilizers. Topical steroids are the main treatment for moderate to severe forms of VKC. However, some patients remain symptomatic despite treatment with topical steroids. Prolonged use of topical steroids may be associated with various complications, such as glaucoma, cataract, and secondary infections. In refractory cases and for avoiding complications related to steroids, immunomodulatory agents such as topical tacrolimus and cyclosporine A are used for the treatment of VKC [8].
Topical tacrolimus 0.05% can help reduce corticosteroid use and is an effective and safe alternative to resistant VKC treatment [7]. Tacrolimus is produced by the fungus streptomyces tsukubaensis. This drug suppresses the immune system and is used to prevent the rejection of transplanted organs. It is a macrolactam derivative with anti-inflammatory and immunomodulatory activities. Tacrolimus binds to an immunophilin and inhibits the enzymatic activity of calcineurin, and therefore, suppresses IL-2 production and T-cell activation [3, 4]. In our case that was resistant to topical steroids, we used the topical tacrolimus 0.05% eye drops that well tolerated and rapidly subsided the inflammation and shrunk the limbal and tarsal papillary hypertrophy.
In our patient, the limbal lesion was due to an allergic inflammatory process that was diagnosed according to IC. As other ocular surface inflammatory conditions such as pterygium, chronic inflammatory cells in the limbus and conjunctiva can damage limbal stem cells [9] as goblet cells seen in corneal IC that revealed to some degree of stem cells damage in our case [10].
The papillary hypertrophic lesions completely healed three months after the topical tacrolimus treatment. Ultimately, the cornea was clear without any conjunctivalization.
In recalcitrant VKC cases, where the symptoms seem to be due to the excessive mass, surgical removal of the lesion can be a therapeutic approach, and it may facilitate resolution of the chronic VKC symptoms [2], but in our patient, the response to topical tacrolimus was so dramatic and rapid that no surgical intervention was needed. Another reason for not having surgery in this patient was the preservation of limbal stem cells.
In this study, we observed that the aqueous formulation of tacrolimus 0.05% is more effective in the steroid-resistant VKC. We found that topical tacrolimus 0.05% was safe and effective in alleviating symptoms and signs of severe VKC that was refractory to topical steroid treatment.
In conclusion, the limbal mass like nodule may be the only obvious manifestation of VKC and should be considered in the differential diagnosis. In a refractory VKC, aqueous formulation of topical tacrolimus can be used and enhance remission in such complex cases and can resolve the patient’s complaints rapidly.
Consent
Written informed consent was obtained from the patient and her parents before the preparation of this case report.
References
- Sangwan VS, Jain V, Vemuganti GK, Murthy SI. Vernal keratoconjunctivitis with limbal stem cell deficiency. Cornea. 2011 May 1;30(5):491-6.
- Kobayashi A, Nagata A, Shirao Y, Kawasaki K, Ohta T, Amaya-Ohkura Y, Nonomura A. Surgical treatment of limbal vernal keratoconjunctivitis by resection of a limbal lesion. Japanese journal of ophthalmology. 2002 Nov 1;46(6):679-81.
- Akbari M, Soltani Moghadam R, Elmi R, Nosrati A, Taghiabadi E, Aghdami N. Topical Tacrolimus as an adjunct to Conventional Therapy for Stromal Herpetic Keratitis: a Randomized Clinical Trial. J Ophthalmic Vis Res. 2019 Oct 24;14(4):400-411. doi: 10.18502/jovr.v14i4.5437. PMID: 31875094; PMCID: PMC6825688.
- Ghasemi H, Djalilian A. Topical Calcineurin Inhibitors: Expanding Indications for Corneal and Ocular Surface Inflammation. J Ophthalmic Vis Res. 2019 Oct 24;14(4):398-399. doi: 10.18502/jovr.v14i5435. PMID: 31875093; PMCID: PMC6825691.
- Chatterjee A, Bandyopadhyay S, Bandyopadhyay SK. Efficacy, Safety and Steroid-sparing Effect of Topical Cyclosporine A 0.05% for Vernal Keratoconjunctivitis in Indian Children. Journal of Ophthalmic & Vision Research. 2019 Oct;14(4):412.
- Akbari M, Elmi R. Herpes simplex virus and human papillomavirus coinfections in hyperimmunoglobulin E syndrome presenting as a conjunctival mass lesion. Case reports in medicine. 2017;2017.
- Kheirkhah A, Zavareh MK, Farzbod F, Mahbod M, Behrouz MJ. Topical 0.005% tacrolimus eye drop for refractory vernal keratoconjunctivitis. Eye. 2011 Jul;25(7):872-80.
- Akpek EK, Dart JK, Watson S, Christen W, Dursun D, Yoo S, O'Brien TP, Schein OD, Gottsch JD. A randomized trial of topical cyclosporin 0.05% in topical steroid–resistant atopic keratoconjunctivitis. Ophthalmology. 2004 Mar 1;111(3):476-82.
- Akbari M, Soltani-Moghadam R, Elmi R, Kazemnejad E. Comparison of free conjunctival autograft versus amniotic membrane transplantation for pterygium surgery. Journal of current ophthalmology. 2017 Dec 1;29(4):282-6.
- Baradaran-Rafii A, Akbari M, Shirzadeh E, Shams M. Single block conjunctival limbal autograft for unilateral total limbal stem cell deficiency. Journal of ophthalmic & vision research. 2015 Jan;10(1):90-2.
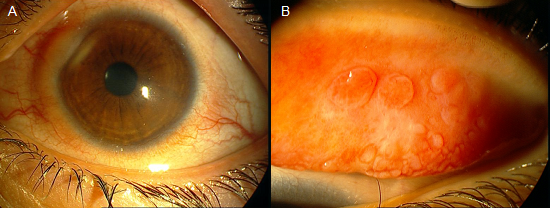
Figure 1(A, B). Solitary limbal nodule and palpebral papillary hypertrophy before treatment with topical tacrolimus
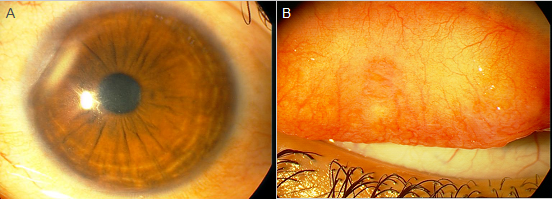
Figure 2(A, B). Limbal nodule and palpebral papillary hypertrophy shrinkage after treatment with topical tacrolimus.
Contact SPER Publications
SPER Publications and
Solutions Pvt. Ltd.
HD - 236,
Near The Shri Ram Millenium School,
Sector 135,
Noida-Greater Noida Expressway,
Noida-201301 [Delhi-NCR] India
